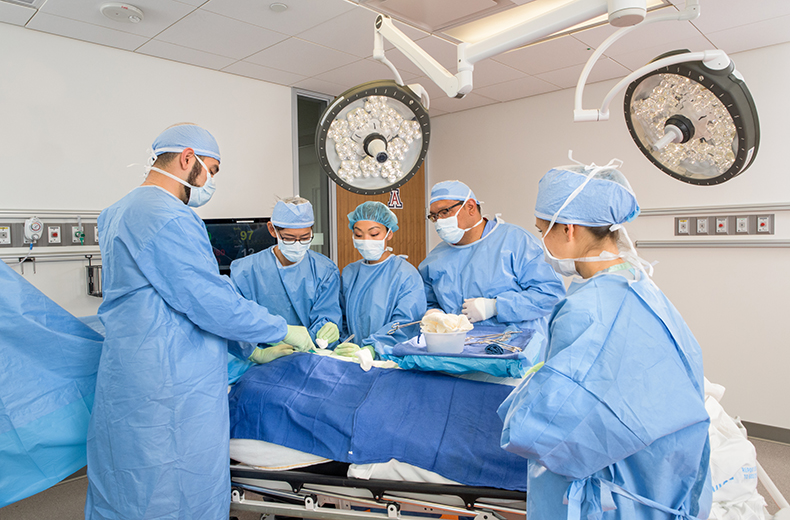
Medical School One of Only Five to Pilot New Surgery Curriculum

The University of Arizona College of Medicine – Phoenix is one of just five medical schools working with the American College of Surgeons and the Association for Surgical Education to pilot a standardized surgery curriculum for third-year students.
Natasha Keric, MD, surgery clerkship director and assistant professor of surgery, is leading the effort at the UA College of Medicine – Phoenix.
The goal is to standardize medical student education in surgery, giving students throughout the country a foundation of knowledge regardless of what specialty they intend to follow, Dr. Keric said. Additionally, the new curriculum will better prepare third-year students for the surgery clinical clerkship exam. This standardized examination, like those in other specialties, is offered by the National Board of Medical Examiners following each clerkship to gauge students’ ability to apply clinical science knowledge to patient problems.
The UA College of Medicine – Phoenix has joined Duke University School of Medicine, Medical College of Wisconsin, University of California San Francisco School of Medicine and Harvard Medical School in piloting the new curriculum.
Steve Lieberman, senior associate dean of academic affairs, said the work being done by Dr. Keric speaks to the constant evolution at the heart of the College of Medicine – Phoenix.
“Dr. Keric personifies the innovation and enthusiasm of the College of Medicine – Phoenix,” Dr. Lieberman said. “Her efforts have led the college to the forefront of innovation in surgical education nationally.”
“Each pilot program is catering the national curriculum to its own curriculum and its own specialties,” Dr. Keric said, explaining how the Phoenix school incorporated simulations. “The bottom line: Will students do better on their shelf exam and will they be more prepared when taking care of surgical patients?”
Previously, students studying for the exam used high-yield books and question banks to test practice, but nobody really knew how to study. “They would read these high-yield books and hope for the best,” Dr. Keric said.
The gratifying part of being involved in the pilot, she said, is the collaboration between the American College of Surgeons, the Association for Surgical Education and the National Board of Medical Examiners.
“It sounds like there is a verbal agreement that they are going to be basing their test off what we’re teaching, which is awesome,” Dr. Keric said.
The process of changing the curriculum has been methodical, with Dr. Keric meeting with representatives from previous classes to ask their opinions on how they study, what they valued in their surgery clerkship, what should change and their top-10 favorite lectures.
“We found that they liked to study independently, they enjoyed simulation, especially those that incorporated what they were learning in the didactics, or core curriculum. And they liked the lectures because it gave them real engaged, face-to-face time with a surgeon who would work through a patient’s case from the start to the operation to post-operative care.”
As a result of the student feedback, didactics were moved to Wednesdays and were coupled with a simulation. The top-10 lectures that they liked were kept and rearranged to fit with a corresponding simulation. The core curriculum was added as the reading didactic portion and is available online, web-based and free.
Among the biggest changes was adding four hours of protected time.
“I wanted to incorporate wellness time,” Dr. Keric said. “That is a culture change for surgeons. There are a lot of misconceptions from surgeons that if you have a day off, you’re not working hard enough or not engaged. The surgery clerkship has a reputation for being difficult because of our high expectations and long hours, and we wanted to focus these as something positive rather than negative. Having some wellness time will recharge the students, keep them engaged and build resilience for them to handle the ‘grit’ of the clerkship.”
Dr. Keric said she is happy with the results so far.
“We are nationally aligned and we have taken input from the students,” she said. “It’s a wonderful blend of what we want from them and what they want from us. I have this new protected time built in for them, which I’m hoping will improve their engagement time when they are on their rotations.”
In addition to their Wednesday didactics, students in the surgery clerkship spend five days on general surgery rotations at hospitals throughout the community, including Banner Medical Centers, Maricopa Medical Center, the VA and several others.
“The ultimate goal (of the surgery clerkship) is for them to learn how to be a doctor and to take ownership of a patient. It’s about quality and not just quantity. It’s learning to utilize all the book knowledge they have gained and apply it clinically to help their patient,” Dr. Keric said.
Representatives from the five pilot programs meet every three months and discuss what’s working and what needs to change. In a year, they will meet and develop a program that other schools can follow, with the knowledge that every medical school clerkship is different.
“Some are four weeks, some six, eight or 12,” Dr. Keric said. “Our how-to will have to be flexible, and with the backing of the American College of Surgeons and the Association for Surgical Education, it won’t be that difficult for other colleges to jump on board.”
Wednesday Surgery Clerkship Didactics and Simulations:
- Week 1: Suturing, knot tying, stapling, nasogastric tube placement, surgical drains and foley catheter placement.
- Week 2: Trauma care and two trauma simulations.
- Week 3: Nutrition in surgical patients and ultrasound simulation.
- Week 4: Acute abdomen/post-operative care and two inpatient simulations.
- Week 5: Gallbladder disease and hepatopancreaticobiliary disease.
- Week 6: Upper GI disease, hernia disease.
- Week 7: Vascular disease, breast disease.
- Week 8: Lower GI disease, endocrine disease.
About the College
Founded in 2007, the University of Arizona College of Medicine – Phoenix inspires and trains exemplary physicians, scientists and leaders to advance its core missions in education, research, clinical care and service to communities across Arizona. The college’s strength lies in our collaborations and partnerships with clinical affiliates, community organizations and industry sponsors. With our primary affiliate, Banner Health, we are recognized as the premier academic medical center in Phoenix. As an anchor institution of the Phoenix Bioscience Core, the college is home to signature research programs in neurosciences, cardiopulmonary diseases, immunology, informatics and metabolism. These focus areas uniquely position us to drive biomedical research and bolster economic development in the region.
As an urban institution with strong roots in rural and tribal health, the college has graduated more than 1,000 physicians and matriculates 130 students each year. Greater than 60% of matriculating students are from Arizona and many continue training at our GME sponsored residency programs, ultimately pursuing local academic and community-based opportunities. While our traditional four-year program continues to thrive, we will launch our recently approved accelerated three-year medical student curriculum with exclusive focus on primary care. This program is designed to further enhance workforce retention needs across Arizona.
The college has embarked on our strategic plan for 2025 to 2030. Learn more.