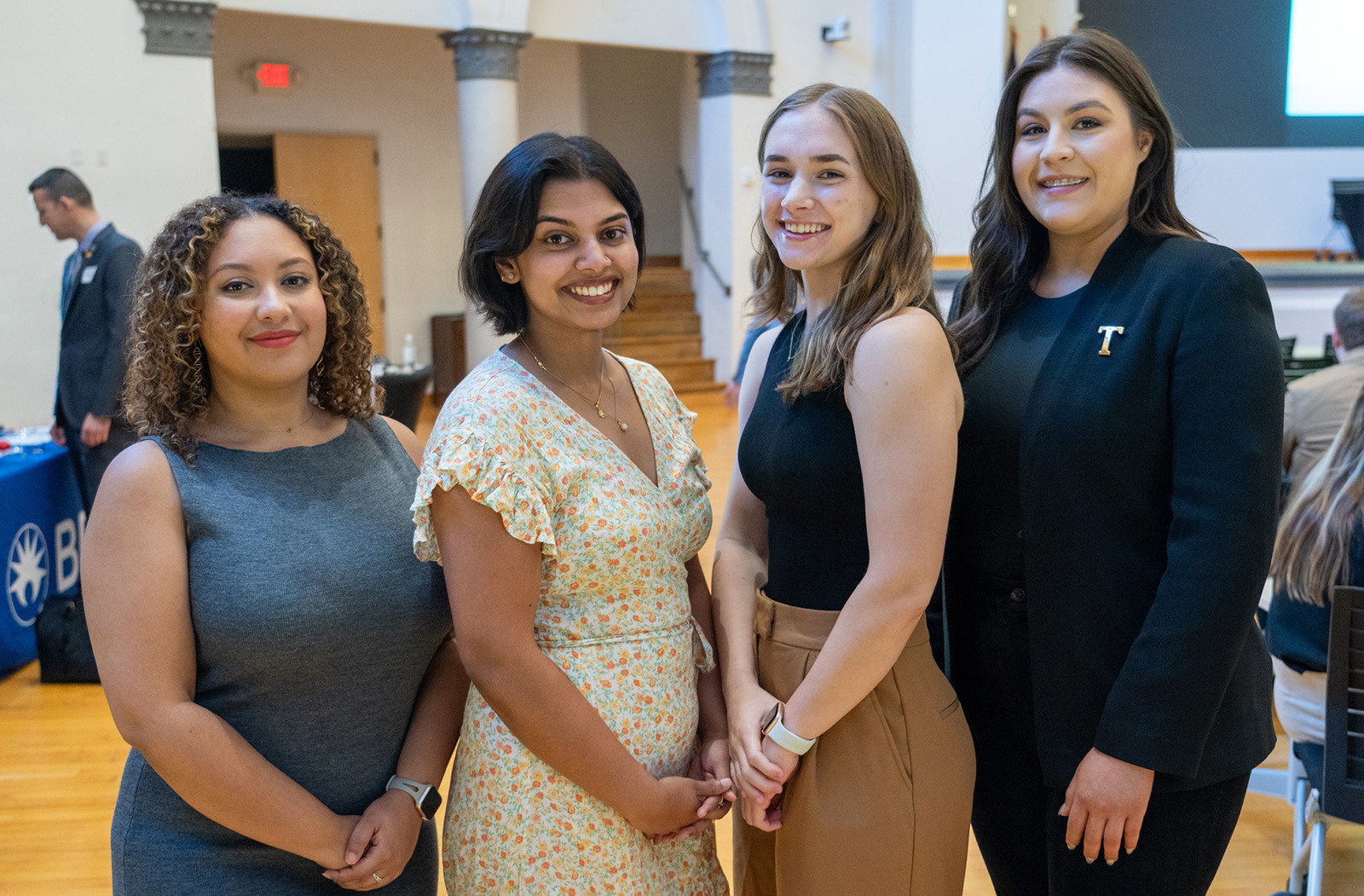
Voice of the Patient
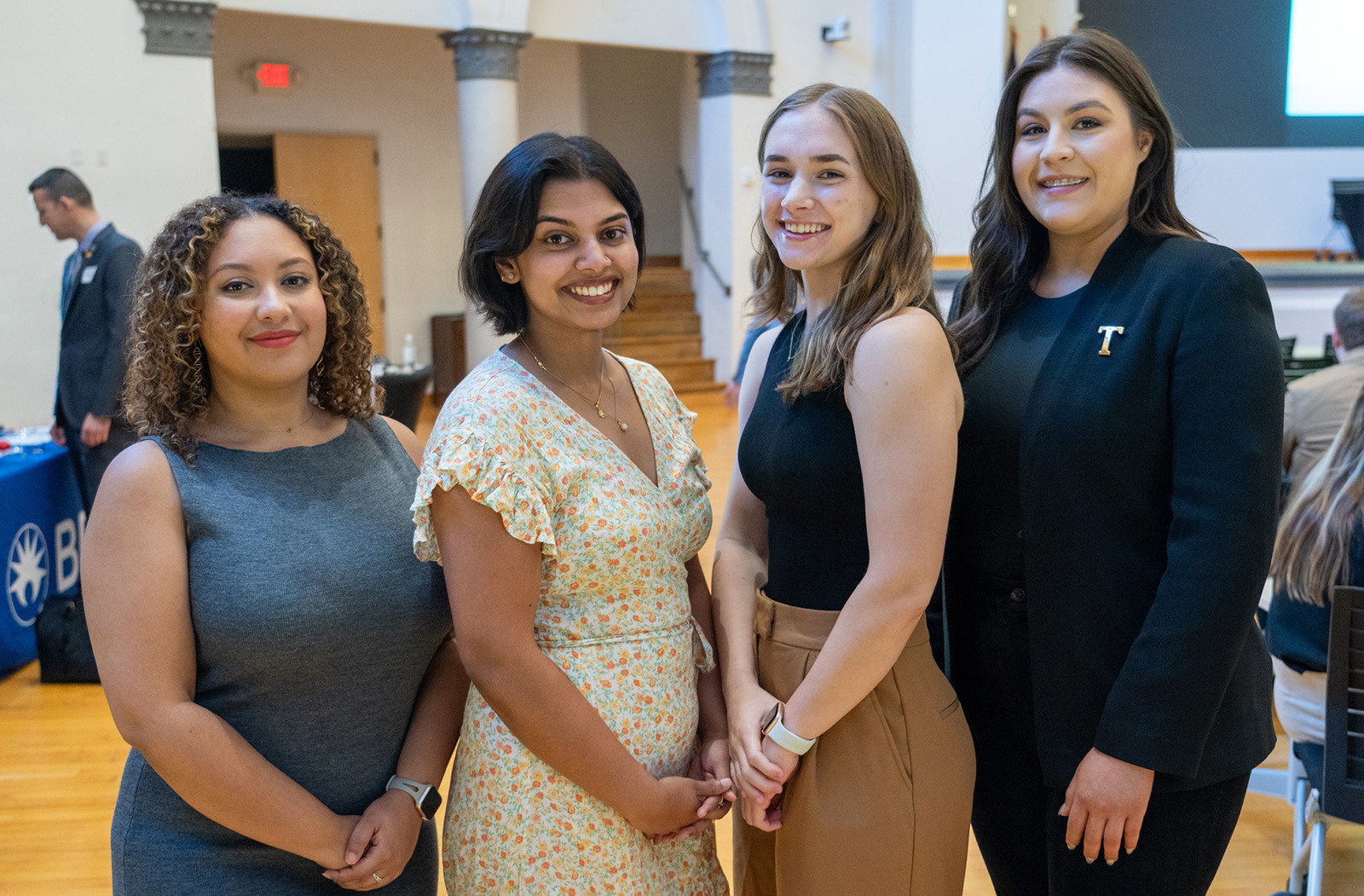
“At some point, we all become a patient.”
This powerful statement came from Alex Tessmer, associate director of Ideation at BD, a medical device company. They were emblematic of the Voice of the Patient event hosted on the University of Arizona College of Medicine – Phoenix’s campus as part of AZBio’s annual Arizona Biosciences Week.
Tessmer participated in a panel titled Patients as Advocates, where he and other patients shared how important it is to be one’s own best advocate. They discussed how engaged physicians can positively impact the lives of their patients, seeking better answers when treatment does not seem to be solving the problem. This last point was further reflected in the narratives of four College of Medicine – Phoenix medical students who shared more about their personal health challenges after the event.

Hoffman was diagnosed with type 1 diabetes when she was just 18-months old and has subsequently been diagnosed with both Hashimoto's disease, a chronic autoimmune disorder that affects the thyroid gland, and rheumatoid arthritis. Her lifelong health struggles have been both humbling and informative.
"Diabetes is a disease that does not behave the same way two days in a row, even when doing the same things every day and sticking to a routine. It fluctuates like the wind, and despite having a forecast, like my continuous glucose monitor, it can be hard to predict,” Hoffman explained. “It has been my greatest teacher while being my biggest adversary. Education and advocacy have become a full-time job in both my personal and professional lives, as I am sure is true for many others.”
Hoffman has come to see diabetes as a way for her to advise people dealing with similar circumstances, and her experiences with doctors — both good and bad — have furthered her desire to become a compassionate, caring physician. She was invited to speak at the event for the second time, having also participated last year.
“When I become a doctor, it will not be my responsibility to pass judgment and make assumptions about my patients. Instead, my job will be to treat my patients and their families as teammates striving toward the same goals, and I will support them in any way I can, all the while adapting to where they are on their journey,” she said.

At a young age, Cherian was diagnosed with an uncommon eye disorder called chronic intermediate uveitis, causing her to temporarily lose her vision. Her frequent visits to the eye clinic served as a strong motivator for her future educational and research work.
“The most important takeaway I got from my physicians was to remember first and foremost that who they see in clinic are people first — not just patients. They have unique wants, needs, concerns and lives; the disease they may suffer from is only part of the equation,” Cherian said. “Each person deserves thoughtful, personalized care. I always want to remember to see my future patients as multifaceted people.”
In addition, Cherian noted that as a physician, it is important to understand the mental and emotional effects of dealing with chronic disease. Not understanding why something is happening or how and when it may get better can take a toll. “I hope that practicing kindness and empathy continue to be increasingly emphasized in medical education,” she said.

She spent time volunteering with the non-profit American Youth Understanding Diabetes Abroad (AYUDA), where she eventually became the director of operations — a position she has held for seven years. Through that organization, she has traveled to the Dominican Republic (DR) on multiple occasions, partnering with a local diabetes foundation to help empower children and adults with diabetes through sustainable diabetes education.
“The inequity in access to medical supplies, treatment and education in the DR was shocking to me at first, but it later became a driving force. I had the same condition as some of these patients, but the health care and education I received were so vastly different that my prognosis and quality of life were significantly better,” Tuomey explained. “I found an aspiration to empower people with illnesses by helping them better understand their conditions and provide the necessary medical education and support to do so.”
Her advocacy work ultimately led her to pursue medicine. Medical school was an avenue to not just educate those with less resources about their condition, but to impact their treatment and care. “As a doctor, I plan to provide my future patients with better knowledge and understanding of their own health to further assist in their wellness, so they can see themselves as more than a diagnosis,” she said.

“After I was diagnosed, I realized how many non-medical factors were barriers to health care, such as insurance, transportation and time,” Walter said. “I became interested in medicine because I am fascinated with human pathophysiology, but I am now interested in addressing these structural and institutional barriers that affect health more than we are able to quantify.”
Walter also expressed gratitude to her doctors for placing her health in high priority. “I was diagnosed in May 2020, right in the height of the early pandemic, and my doctor managed to get me into her office to get bloodwork, despite my fever. I credit her with saving my life because she went the extra mile for me, even though we had just met,” she said.

The dogged determination to stay on top of best practices and his willingness to go above and beyond to get her the medications she needs helped Walter to understand the type of physician she wants to be.
Each participant’s story was a testament to how important it is for a patient to feel heard and for a physician to truly listen — a sentiment Kevin Lohenry, PhD, PA-C, interim dean of the College of Health Sciences at the University of Arizona, stressed in his opening remarks. “Collectively, we can make the world a better place. You can be better advocates; we can educate patients and the community about bioscience and truly engage with patients and their family in their health and wellness.”
About the College
Founded in 2007, the University of Arizona College of Medicine – Phoenix inspires and trains exemplary physicians, scientists and leaders to advance its core missions in education, research, clinical care and service to communities across Arizona. The college’s strength lies in our collaborations and partnerships with clinical affiliates, community organizations and industry sponsors. With our primary affiliate, Banner Health, we are recognized as the premier academic medical center in Phoenix. As an anchor institution of the Phoenix Bioscience Core, the college is home to signature research programs in neurosciences, cardiopulmonary diseases, immunology, informatics and metabolism. These focus areas uniquely position us to drive biomedical research and bolster economic development in the region.
As an urban institution with strong roots in rural and tribal health, the college has graduated more than 1,000 physicians and matriculates 130 students each year. Greater than 60% of matriculating students are from Arizona and many continue training at our GME sponsored residency programs, ultimately pursuing local academic and community-based opportunities. While our traditional four-year program continues to thrive, we will launch our recently approved accelerated three-year medical student curriculum with exclusive focus on primary care. This program is designed to further enhance workforce retention needs across Arizona.
The college has embarked on our strategic plan for 2025 to 2030. Learn more.